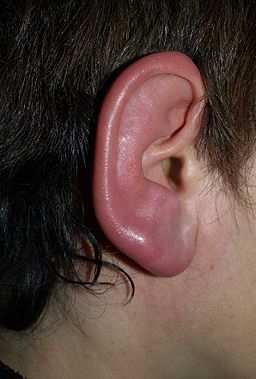
This is the effect of the skin condition on the ear lobe – swollen and painful
Image Klaus D. Peter, Gummersbach, Germany (Own work) [CC-BY-3.0-de (https://creativecommons.org/licenses/by/3.0/de/deed.en)], via Wikimedia Commons
What Causes Erysipelas?
The infection is caused and spread by excessive colonisation of the Streptococcus bacteria, particularly where skin wounds are present. People with existing skin disorders such as ulcers and eczema are at higher risk of erysipelas.
Streptococcus may set in after skin injury including cuts and scrapes, dog or insect bites and following surgery. We may naturally have a presence of the bacteria in our body, but the bacteria will become harmful if over-colonisation is allowed, spreading infection, toxaemia and sepsis.
Editor’s note: You will find the following video helpful for understanding the causes of this skin condition and the best ways of treating it.
Who is at Risk of Getting Erysipelas?
Babies, children and senior persons are at higher risk of contracting streptococcus as their immune systems are naturally weaker. People with weak immunity or immune disorders, impairments of the venous system, diabetes and alcoholism conditions are also at high risk of infection.
Similarly, those who have had surgeries such as gastric bypass, mammography or pelvic operations are at higher risk of the streptococcus infection and erysipelas conditions. People with existing skin conditions such as ulcers or fungal infections are also at greater risk, as are those with lymph drainage disorders that prevent healthy circulation to the skin.
What are the Symptoms of Erysipelas?
The symptoms of Erysipelas usually present about 48 hours after streptococcus infection, and include:
- Skin lesion or rash
- Warm, inflamed and blistered skin
- Headaches
- Fever
- Vomiting
- Fatigue
The body extremities such as the fingers and toes, limbs and face are prone to erysipelas. People often get the rash on their arms or legs shortly after infection. The streptococcus infection may spread through fatty tissue causing a hard, raised rash around the cheeks, ears and eyes. Fluid may ooze from the lesion, but it is generally without pus.
Symptoms may range from mild to severe and develop into sepsis and necrotizing lesions as the infection spreads through the bloodstream. Receiving medical attention as soon as possible is essential to prevent the infection spreading throughout the body and causing other health complications, especially affecting lymph drainage, valve function and bone joints.
How is Erysipelas Diagnosed?
A physical examination of the skin lesions may be enough to diagnose the condition, as the skin appearance is quite unique to erysipelas. A titer called antistreptolysin O (ASO) may be used to confirm diagnosis, but a skin biopsy is usually not necessary. Blood tests may confirm the presence of sepsis.
Editor’s note: This skin condition is very similar to Cellulitis and the two terms are often used interchangeably. However, Cellulitis affects lower, deeper levels of the skin whereas Erysipelas affects layers closer to the surface.
How is Erysipelas Treated?
Treatment varies according to the severity of the infection and how far it has spread. Typical treatments include:
- Penicillin
- Antibiotics, including Prophylactics
- Erythromycin
- Clindamycin
Medications may be administered orally or intravenously depending on the degree of streptococcus infection and its impact on the body. Symptoms such as headaches, fever, vomiting and fatigue should subside within a 48 hour period after commencing treatment.
The erysipelas skin lesions may only heal after a fortnight and the skin can peel during this time. Re-infection is possible and so it is important to complete the course of treatment prescribed. In about 30 per cent of cases re-infection occurs after treatment.
How does Erysipelas Impact Overall Health?
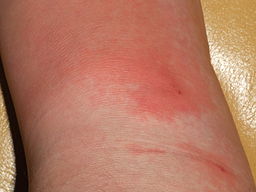
Image by Poupou l’quourouce (Own work) [GFDL (https://www.gnu.org/copyleft/fdl.html), CC-BY-SA-3.0 (https://creativecommons.org/licenses/by-sa/3.0/) or CC-BY-SA-2.5-2.0-1.0 (https://creativecommons.org/licenses/by-sa/2.5-2.0-1.0)], via Wikimedia Commons
How is Erysipelas Prevented?
Prevention is often performed by making sure you do not get infected with the streptococcus bacteria. Such infection may be prevented through avoiding skin injuries and sores, and by keeping the skin clean, hydrated and healthy. Receiving immediate medical attention once symptoms presents allows early treatment to prevent spread of the infection, septic shock and impacts on health.

